By Kelly A. Reynolds, MSPH, PhD
A proactive approach is needed to effectively manage indigenous microbes in tap water supplies. Microbes such as Legionella, Mycobacterium, Pseudomonas and various free-living amoeba are naturally present in tap water and increase in concentration exponentially under the right growth conditions. Failure to be proactive has resulted in adverse human health effects, including severe illness and death, as well as costly litigation. Studies indicate that 10-40 percent of hospital-acquired pneumonias are Legionnaire’s disease and that from 2011-2012, 67 percent (14/21) of Legionella outbreaks and 86 percent (12/14) of outbreak-associated deaths were in healthcare facilities.(1) While POU devices offer solutions at the tap, the need for proper maintenance and cost effectiveness must be carefully considered.
A proactive approach
Over the last decade, increases in Legionella outbreaks have spurred numerous media headlines:
“Warning that ‘warm water’ systems in apartment buildings pose Legionella risk.” www.theage.com.au/national/investigations/warm-water-systems-in-apartment-buildings-a-legionella-risk-20161201-gt1mxl.html. Melbourne’s The Age. 12/4/2016
“Prison aware of Legionella in water.” http://triblive.com/local/allegheny/11501687-74/department-legionella-cooling. Pittsburgh Tribune-Review. 11/20/2016
“Flint water likely Legionella cause, expert says.” www.detroitnews.com/story/news/michigan/flint-water-crisis/2016/12/04/flint-water-switch-bacteria-legionnaires/94979698/. The Detroit News. 12/06/2016.
“Gardeners warned as Legionella infections spike in Marlborough.” www.stuff.co.nz/national/health/87381767/gardeners-warned-as-legionella-infections-spike-in-marlborough. Fairfax Stuff. 12/09/2016.
This outbreak surge and increased awareness has prompted government agencies and industry stakeholders to release numerous directives on legionellosis prevention training, reporting and response. Recently, the Centers for Disease Control (CDC) issued a new guide and toolkit, Developing a Water Management Program to Reduce Legionella Growth and Spread in Buildings: A Practical Guide to Implementing Industry Standards(2) and have teamed with the National Network of Public Health Institutes and researchers at the University of Arizona to create a user-friendly online training aimed at proactive Legionella monitoring and control that will be available by fall 2017.
Larger-building water systems, such as those in hospitals, require a proactive treatment approach but have competing priorities. Reduced energy costs and increased safety against scalding are benefits of maintaining lower hot-water system temperatures but can create a more favorable environment for bacterial growth. Optimal temperature for hot water is > 51°C (124°F), which requires a setting of 60°C (140°F) to maintain high temperatures throughout the premise plumbing. Responsibilities for system maintenance may include facility managers or administration, infection preventionists or environmental services personnel. Building design, water-use patterns, stagnation zones, patient vulnerabilities and treatment practices may be unique to specific sites. Therefore, site-specific assessments of critical control points and optimal treatment zones are essential for developing an effective management plan.
Water safety plan development
A review of current practices in Legionella prevention reveals training gaps for environmental health professionals. Recent recommendations from the World Health Organization (WHO), CDC and the American Society of Heating and Air-Conditioning Engineers (ASHRAE) represent a shift toward increased responsibility for facilities to manage contamination risks by developing a water safety plan for individual sites. The first step in developing such a plan is to understand Legionella characteristics, transmission and incidence, risk-assessment tools and control options matched with site-specific environmental characteristics of influence.
While development of a water safety plan is critical for legionellosis prevention, even well-maintained systems can harbor the harmful bacteria. Zones of stagnation or biofilm growth are common in premise plumbing and difficult to control. Thus, a multi-barrier approach to prevent Legionella exposures is necessary. Regardless of controls put in place, monitoring is required to determine water quality and safety. Routine monitoring can help to determine whether controls are effective or if changes in water distribution variables contribute to an increase in bacterial concentrations.
The CDC has not established a safe level of Legionella and positive results are likely due to the nature and ubiquity of the organism. The presence of Legionella does not automatically mean there are adverse health effects or an outbreak occurring. The balance between environmental concentration, infectious dose, exposure probabilities and host susceptibility are in a complex balance regarding disease manifestation.
 POU treatment benefits
POU treatment benefits
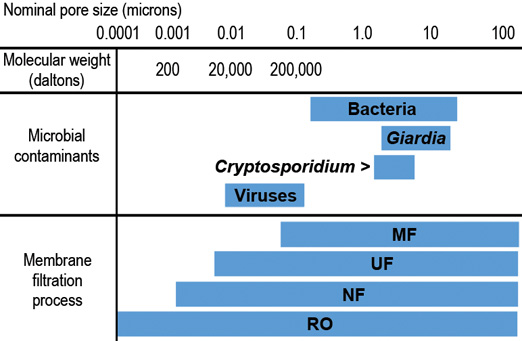
As a final barrier to reducing the risks of Legionella and other indigenous pathogen exposure, POU filtration devices have been incorporated into targeted water safety plans. Filtration technologies capable of removing Legionella include microfiltration (MF), ultrafiltration (UF), nanofiltration (NF) and reverse osmosis (RO). Figure 1 shows a comparison of filtration technologies, particle sizes and molecular weight cut-off limits.
Legionella cells measured from laboratory cultures range from 0.3-0.9 um wide and 2-20 um long (WHO, 2007) and thus a variety of filtration options is available for removal of bacteria from tap-water supplies. POU filtration offers an effective approach for residential and large-scale (i.e., schools, hospitals, hotels, long-term care facilities) water system treatment, either for proactive maintenance or emergency response.
Research has shown that POU treatment in hospital wards with patient populations at high risk for water-related infections is especially beneficial. For example, a study of water-related bacterial infections in a sub-acute care unit in a 208-bed medical center found POU water filtration to significantly and cost-effectively reduce the risk of Legionella colonization and infection.(4) In this same study, 28 percent (6/21) of unfiltered tap-water samples tested positive for water-based pathogens compared to zero percent (0/42) of filtered water samples. A 90.2-percent, statistically significant reduction in patient colonization rates (resulting in a net savings of $231K in patient care costs) were also documented.
POU devices are certified for removal of microbes relative to the appropriate ANSI standard (Standard 53: Drinking Water Treatment Units–Health Effects and Standard 58: Reverse Osmosis Drinking Water Treatment Systems). While numerous studies have shown POU-filtration success for controlling Legionella in hospital systems, they are usually implemented as part of an overall disinfection treatment plan and are commonly referred to as an emergency remediation action along with system flushing, super-heating the water and shock chlorination. Few feasibility studies where POU devices are used routinely as a management solution have been reported but with recommended filter replacement every four to eight weeks, routine use of the method could be very costly.(3) Furthermore, biofilm growth and increased counts of general bacteria (i.e., heterotrophic plate count) must be managed in the POU devices via frequent filter changes or other antibacterial treatments. Improper maintenance of POU devices cannot be tolerated, as this may result in concentration of bacteria, membrane fouling and increased exposures as biofilm eventually slough off. While following manufacturer’s instructions for proper use and maintenance is critical, US EPA further provides guidance on POU device operation and maintenance. In that document, examples of maintenance logs are provided for tracking flows, replacement needs/rates and inspection of mechanical warning devices for routine part replacement/repair.(5)
Conclusions
Overall, control of premise-plumbing contamination is now generally accepted to be the responsibility of the facility owner or manager. Given the variability of systems, there is a need for site-specific assessments of risk and appropriate water management or safety plans. While POU devices offer effective management of Legionella and other bacteria contaminating distribution systems, evaluation of cost-effectiveness, efficacy and feasibility need further exploration.
References
(1) Beer, KD, Gargano, JW, Roberts, VA, et al. Surveillance for Waterborne Disease Outbreaks Associated with Drinking Water – United States, 2011-2012. MMWR Morb Mortal Wkly Rep. 2015;64(31):842-848. www.ncbi.nlm.nih.gov/pubmed/26270059. Accessed June 20, 2016.
(2) CDC. Developing a Water Management Program to Reduce Legionella Growth & Spread in Buildings: A Practical Guide to Implementing Industry Standards, 2016. www.cdc.gov/legionella/maintenance/wmp-toolkit.html.
(3) US EPA. Technologies for Legionella Control in Premise Plumbing Systems: Scientific Literature Review, 2016. https://www.epa.gov/sites/production/files/2016-09/documents/legionella_document_master_september_2016_final.pdf. Accessed December 14, 2016.
(4) Holmes C, Cervia JS, Ortolano GA, Canonica FP. Preventive Efficacy and Cost-Effectiveness of Point-of-Use Water Filtration in a Subacute Care Unit. Vol 38, 2010. doi:10.1016/j.ajic.2009.04.284.
(5) US EPA. Point-of-Use or Point-of-Entry Treatment Options for Small Drinking Water Systems. Arlington, VA; 2006.
 About the author
About the author
Dr. Kelly A. Reynolds is an Associate Professor at the University of Arizona College of Public Health. She holds a Master of Science Degree in public health from the University of South Florida and a doctorate in microbiology from the University of Arizona. Reynolds is WC&P’s Public Health Editor and a former member of the Technical Review Committee. She can be reached via email at [email protected]





