By Kelly A. Reynolds, MSPH, PhD
Arsenic is naturally occurring in soil and rocks throughout the US and readily dissolves into water, particularly groundwater supplies. Exposure to arsenic via inhalation, ingestion and skin absorption can lead to cancers of the lung, bladder and skin. The estimated disease burden cost of known arsenic-related cancers in the US is $1.6 billion per year. Adverse outcomes other than cancers, including diabetes, cardiovascular disease, affected pregnancy and child development outcomes, as well as skin lesions, have also been suggested.(1) The lack of a perceived problem, testing by well owners and controversy of risks at low-dose exposures contribute to a reduced concern over arsenic exposures that may otherwise be preventable.
Who should test for arsenic?
In the US, an estimated 43 million Americans utilize private wells as their drinking water source. Identification of arsenic contamination in household wells is difficult, given there is no federal oversight and no mandatory monitoring of these private sources. Arsenic in water has no taste or smell; therefore, homeowners may not perceive a problem with their water and thus, are generally not motivated to invest time and money for testing.
Monitoring and treatment costs are inherent barriers for the primarily rural populations at risk. Such barriers are particularly significant deterrents in lower-income households. In one study, families from households (n = 188) in Montana and Washington with income levels below the federal poverty level reportedly never tested their water or considered taking additional precautions. Water testing in these same households showed that nearly 27 percent of homes tested positive for at least one regulated contaminant at levels above a US EPA maximum contaminant limit (MCL). Contaminants and their isolation frequency above the MCL included: total coliforms (18 percent), arsenic (six percent), synthetic organic chemicals (six percent), nitrates (two percent), fluoride (two percent) and Escherichia coli (< one percent).(1)
US EPA has set an upper limit for inorganic arsenic in municipal water at 10 µg/L (10 ppb). Surveys from the US Geological Survey’s National Water Information System (NWIS) and others have found that nearly half of the 30,000 positive arsenic samples they collected from US waters (private and public) were below concentrations of one µg/L. Ten percent (mostly in the western US) however, exceeded 10 µg/L.(2) Arizona and Nevada consistently reported the highest median and maximum values compared to other states.
Monitoring arsenic levels in water
Arsenic concentrations in groundwater are relatively persistent over time due to the natural dissolving properties of the contaminant from surrounding rock formations. Thus, historical concentration values are assumed to remain constant over time. Select wells are monitored for arsenic throughout the US via the National Ground-Water Monitoring Network (NGWMN) as required by the Subcommittees on Groundwater of the Federal Advisory Committee on Water Information (ACWI). The monitoring database provides over 15 years of information on arsenic concentrations, well construction, water levels and quality, and regional rock formations.
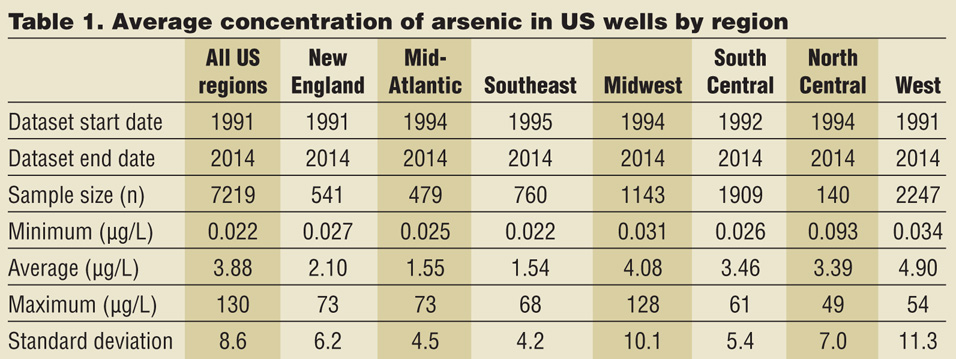
Based on a collection of over 7,000 public and private groundwater wells tested, arsenic concentrations ranged from 0.1 to 130 µg/L with a US average of 3.88 µg/L (3) (see Table 1). The highest average concentrations of 4.9 µg/L were in the western US region, as expected.
 Are low dose exposures hazardous?
Are low dose exposures hazardous?
According to US EPA toxicological risk evaluations of arsenic, a risk probability of one in 20,000 is estimated for every µg/L of arsenic with risk increasing linearly in relationship to dose. Using these estimates, even low levels of arsenic in water are considered problematic. Estimating the risk of arsenic exposures at low-dose concentrations (common to US waters), however, is a controversial issue.
Well-known are the high-dose exposures in Taiwan, Chile and Bangladesh, exceeding the US EPA MCL a hundred-fold or more. Studies vary on whether or not there is a threshold exposure value below which arsenic is not harmful. Merely finding arsenic in water may not directly infer unacceptable risks. While there is some evidence for the threshold theory in laboratory rodents, the effect in humans may not be the same, prompting regulatory scientists to err on the side of safety and assume there is no dose threshold. The National Research Council has been critical of the US EPA’s method for risk assessment related to arsenic exposures, suggesting that early-life exposures, even at low concentrations, present unacceptable risks. These risks are greater for many vulnerable populations, such as children and pregnant women or those suffering from chronic illnesses.
Given that arsenic is ubiquitous in nature, setting low regulatory limits that are achievable can be a challenge.(4) Food is also a large source of arsenic exposure, where residual arsenical herbicides contaminate items like rice and apple juice. Use of arsenical herbicides in soil crops and as feed additives is being phased out but still make their way into the food chain.
Water treatment options
Extrapolation of arsenic low-dose effects from high-dose exposures may be inherently flawed but the real risk remains unknown. Risk estimates are further complicated by whether or not the necessary reactive arsenic metabolites are generated to react with and damage cellular proteins. Generation of the reactive metabolites may vary based on genetics, diet and individual behaviors, such as smoking.
Private water supplies should follow the lead of municipalities and remove arsenic from drinking water prior to consumption to below the 10 µg/L MCL. Arsenic removal efficiency at public water treatment plants ranges from 12 to 44 percent, while targeted POU devices achieve an overall greater result.(5) A recent study in a small community in the southwestern US found that POU devices removed up to 99 percent of arsenic concentrations.(6)
The ability of POU devices to remove arsenic in water depends on many variables, including pH and redox potential, which control arsenic speciation and thus drive treatment options. Activated carbon has been studied extensively for arsenic removal but carbon only removes a few milligrams of metal ions per gram of activated carbon.(7) Other popular treatment options include reverse osmosis, adsorptive media (e.g., iron-based media and alumina) and distillation. Consumers should target POU devices certified for arsenic reduction as per American National Standards Institute (ANSI) and National Sanitation Foundation (NSF) criteria related to removal via reverse osmosis (Standard 58); adsorptive media (Standard 53) or distillation (Standard 42). Certified devices have been tested for minimum reduction capacity at high arsenic influent concentrations in public or private drinking water.
References
(1) Zheng Y, Ayotte JD. At the Crossroads: Hazard Assessment and Reduction of Health Risks from Arsenic in Private Well Waters of Northeastern United States and Atlantic Canada HHS Public Access. Science of the Total Environment Febr. 2015;1(505):1237-1247. doi:10.1016/j.scitotenv.2014.10.089.
(2) Welch AlH, Westjohn DB, Helsel DR, Wanty RB. Asrenic in ground water in the United States: Occurrence and Geochemistry. Ground Water. 2000;38(4):589-604.
(3) USGS National Water Quality Assessment Data Warehouse. 2015. US Geological Survey. http://cida.usgs.gov/nawqa_www/nawqa_data_redirect.html?p=136:1:0. Accessed June 1, 2015.
(4) Schmidt CW. Low-Dose Arsenic: In Search of a Risk Threshold. Environmental Health Perspectives. 2014;122(5):A130-A134. doi:10.1289/ehp.122-A130.
(5) Frey MM, Edwards MA. Surveying arsenic occurrence. Journal of the American Water Works Association. 1997;89(3).
(6) Lothrop N, Wilkinson S, Verhougstraete MP, et al. Home Water Treatment Habits and Effectiveness in a Rural Arizona Community. Water. 2015;7(3):1217-1231. doi:10.3390/w7031217.
(7) Mohan D, Pittman CU. Arsenic removal from water/wastewater using adsorbents–A critical review. Journal of Hazardous Materials. 2007;142(1-2):1-53. doi:10.1016/j.jhazmat.2007.01.006.
 About the author
About the author
Dr. Kelly A. Reynolds is an Associate Professor at the University of Arizona College of Public Health. She holds a Master of Science Degree in public health (MSPH) from the University of South Florida and a doctorate in microbiology from the University of Arizona. Reynolds is WC&P’s Public Health Editor and a former member of the Technical Review Committee. She can be reached via email at [email protected]





